Medicaid redetermination is often framed as an eligibility issue—but in practice, it is primarily a communication and member engagement challenge. In reality, many members are losing coverage for a very different reason: they simply lack clear guidance on what to do — or when they need to do it.
Medicaid redetermination is the process by which states verify whether individuals remain eligible for Medicaid coverage, requiring members to confirm information and complete renewal steps within a defined timeframe.
Members miss redetermination deadlines, fail to provide required paperwork, or misunderstand other requirements. In many cases, the problem causing them to lose their coverage is not eligibility. It is communication gaps.
During the Medicaid unwinding period, approximately 71% of disenrollments were procedural— meaning members remain eligible but lose coverage because required administrative steps were not completed correctly. While more recent reporting varies across states, procedural disenrollment remains a significant driver of coverage loss across Medicaid populations. These rates improved following the unwinding period but are expected to decline again under new H.R. 1 requirements.
This results in preventable membership loss, revenue erosion, increased call center burden, and disruption to quality and care management programs and critical outcomes.
Procedural disenrollment is fundamentally a member engagement problem. Procedural disenrollment occurs when eligible Medicaid members lose coverage because they do not complete required administrative steps. When members are not clearly guided through the renewal process, they cannot complete it successfully.
Solving that communication challenge at scale is achievable with the right approach, and the right tools. For health plans, improving Medicaid redetermination outcomes is directly tied to member retention, revenue stability, and regulatory performance.
Why Redetermination Engagement Is So Difficult
Health plans and States must reach millions of members and guide them through a time-sensitive eligibility process that involves multiple steps, documents, and deadlines.
The difficulty is not simply sending reminders. The first challenge is in actually reaching members when contact information is often out of date. The next challenge is engaging members with specific guidance on what actions they need to take to retain coverage.
Common barriers to Medicaid redetermination engagement include:
- Member contact information is often incomplete or outdated
- Communication channels may be limited or regulated
- Outreach must occur at precisely the right times in the redetermination cycle
- Messages must clearly explain what action members must take, and provide support resources when needed
In other words, alert communications are not enough — members need to be guided and supported through the process by the State, the MCO, providers and community resources.
With many members having a smart phone as their primary means of communication and technology access, digital engagement can play a powerful role in this effort. Scaling communication across an entire population introduces another challenge: regulatory compliance.
The Compliance Challenge in Digital Engagement
Compliant digital engagement refers to communication workflows that follow regulatory requirements, utilize approved messaging, and deliver auditability at every step of the member interaction.
As plans scale digital engagement, the challenge is not just increasing outreach — it is ensuring members receive clear, actionable direction and complete the necessary steps to retain coverage. Health plans must provide step-by-step instructions, deadlines, and required documents in each communication.
This is especially important because Medicaid redetermination is a regulated eligibility process. Communications are subject to federal and state oversight, mandated disclosures, accessibility standards, and audit requirements. Every message must be correct, compliant, and aligned to where the member is in the process — while still making the next step explicit and easy to follow.
At population scale, engagement workflows must:
- Enforce policy-aligned, pre-approved language
- Deliver required disclosures consistently across channels
- Log and preserve interactions for audit review
- Protect PHI and eligibility data
- Maintain continuity across digital and assisted channels
- Guide members through each step of the process with clarity, not just notify them that action is required
Without these controls, automation may increase speed while simultaneously increasing regulatory risk. In a regulated environment, that is not just inefficient — it is unacceptable. It can also increase confusion — leading to missed deadlines, incomplete submissions, and preventable loss of coverage.
This is where compliance becomes essential.
What Compliant Digital Engagement Looks Like
Plans that navigate redetermination successfully are not increasing outreach — they are redesigning how communication works. They are designing communication strategies that give members clear direction on what’s required, when to act, and how to complete each step.
That typically includes:
- Policy-aligned messaging frameworks that prevent unauthorized language drift
- Guardrails that constrain communications within approved parameters
- Full interaction traceability and replay capability
- Human-in-the-loop escalation for sensitive or complex scenarios
- Secure data access aligned with least-privilege principles
- Clear, consistent guidance that reinforces next steps across every interaction
These capabilities allow plans to scale communication and guidance while maintaining compliance integrity. They also ensure members are not just contacted, but effectively supported through the process.
In other words, compliance is possible in redetermination communications.
Compliance Must Be Embedded, Not Added Later
Compliance in Medicaid redetermination cannot exist solely as documentation or after-the-fact audit review. It must be built into the runtime of the engagement platform itself. Regulatory requirements and clarity must be enforced at the moment communication happens — not retroactively.
That means:
- Compliance rules enforced when messages are generated
- Guardrails that constrain responses and messaging before they reach members
- Version control tied to approved disclosure language
- Full interaction replay available for audit review
- Continuous monitoring of system behavior
- Built-in controls that ensure every interaction remains accurate, consistent, and actionable
This approach transforms governance from oversight into operational infrastructure. It ensures that as engagement scales, communication quality and regulatory integrity do not degrade.
Ushur’s Agentic CX platform was built specifically for regulated industries where every interaction may be subject to regulatory review. Rather than adding compliance and governance controls after deployment, Ushur embeds runtime guardrails, traceability, and controls directly into engagement workflows. This allows plans to scale digital engagement while maintaining confidence that every interaction is compliant, accurate and clearly guides member action.
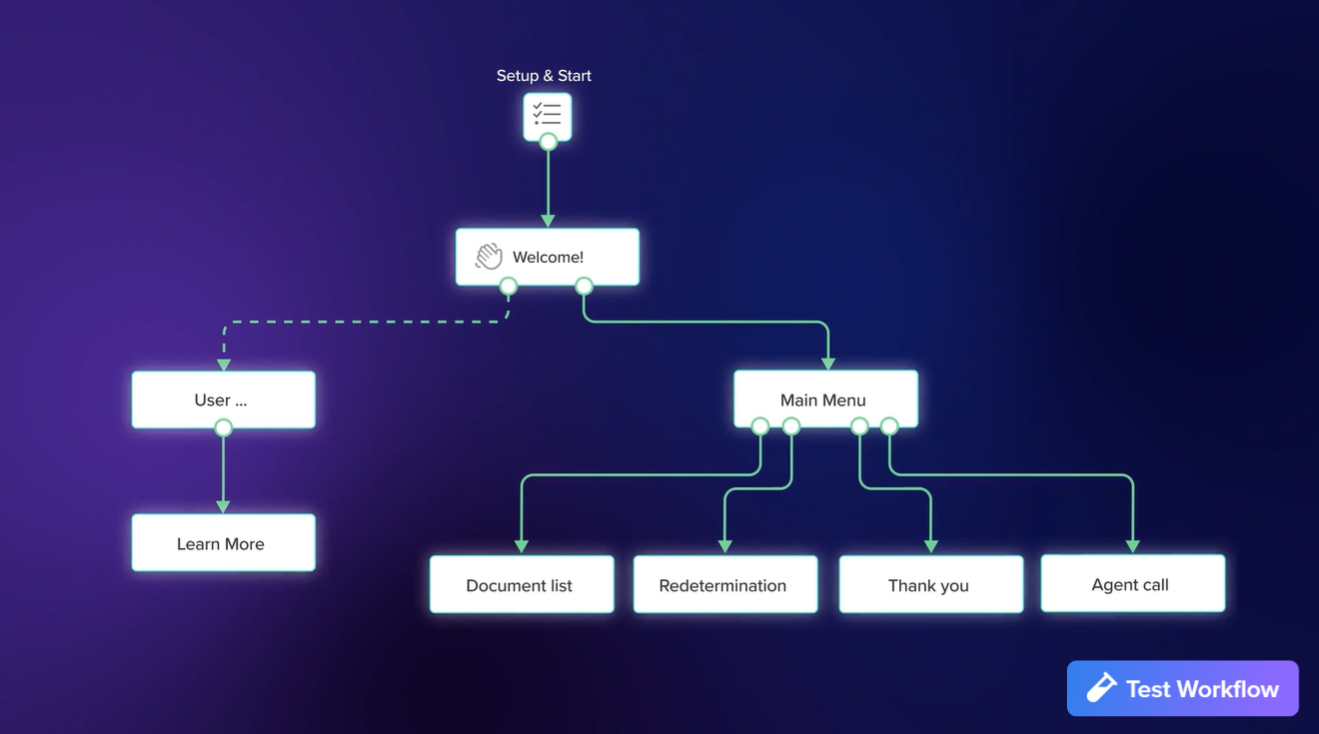
One example of this in practice is Ushur’s Voice-Guided Experience for Medicaid Redetermination, which combines AI-powered voice interaction with a synchronized mobile interface to guide members through renewal steps in real time. Members stay on the call while following secure visual prompts, making it easy to confirm contact information, update details, and complete required actions without friction.
In Medicaid redetermination, the difference between simply notifying members and actively guiding them through completion is what drives outcomes.
Additional Resource for Health Plans Navigating Redetermination
For health plans looking to operationalize digital engagement during redetermination, Ushur recently published a comprehensive guide outlining strategies for reducing procedural disenrollment while maintaining compliance and audit readiness.
The guide explores how plans can combine digital engagement, automation, and governance controls to deliver clear, consistent, and compliant guidance that helps members complete the renewal process successfully.
Download Overcoming Medicaid Eligibility & Redetermination Hurdles: The 2026 Guide to Continuous Enrollment & Medicaid Member Retention to learn how leading plans are navigating redetermination engagement at scale while improving member understanding and reducing preventable loss of coverage.
Reducing Preventable Member Loss
The objective of Medicaid redetermination outreach is clear: protect eligible members, reduce avoidable churn, stabilize revenue, and maintain trust with regulators and stakeholders.
Achieving that objective requires more than communication volume. It requires communication that helps members understand the process and successfully complete required actions.
Many members do not lose coverage because they are ineligible — they lose it because they do not understand what to do or do not complete required steps in time.
Digital engagement can play a meaningful role in this effort, but its effectiveness depends on whether it reduces confusion and supports completion — not just increases outreach.
How health plans can reduce procedural disenrollment:
- Provide step-by-step renewal instructions
- Send reminders tied to deadlines
- Enable digital document submission
- Guide members through each step in real time
- Amplifying member outreach within procedural disenrollment grace period
Redetermination is fundamentally about helping members complete the renewal process. When communication provides step-by-step direction — and drives members to take needed actions — plans can reduce procedural disenrollment while maintaining regulatory confidence.
Medicaid redetermination is not just an eligibility issue—it is a communication and engagement challenge. Health plans that provide clear, step-by-step guidance and compliant digital experiences can reduce procedural disenrollment, improve member retention, and maintain compliance at scale.
Frequently Asked Questions about Medicaid Redetermination Engagement
Q1. How can health plans measure whether their redetermination engagement strategy is working?
Plans should track renewal completion rates, procedural disenrollment rates, and member response times to outreach—not just message volume, but whether members understand what to do and successfully complete required steps.
Q2. What role does digital member experience play in Medicaid retention?
Digital engagement should help members understand what is required of them and complete renewal steps, providing specific, easy-to-follow guidance, support and resources to reduce confusion and missed deadlines.
Q3. How does the H.R.1 law change the redetermination landscape for health plans?
H.R.1 increases the frequency and complexity of eligibility checks, requiring plans to support more frequent renewal cycles and clearer member communication, making it critical that communication is consistent, accurate, and helps members take the right action at the right time. It also introduces new work requirements as part of eligibility.
Q4. What should health plans look for in a digital engagement platform for redetermination?
Plans need platforms that combine multi-channel engagement with built-in compliance controls, auditability, and governance, while ensuring communication remains clear, consistent, and guides members through the process from start to finish.