The AI Agent-powered CX platform for regulated industries
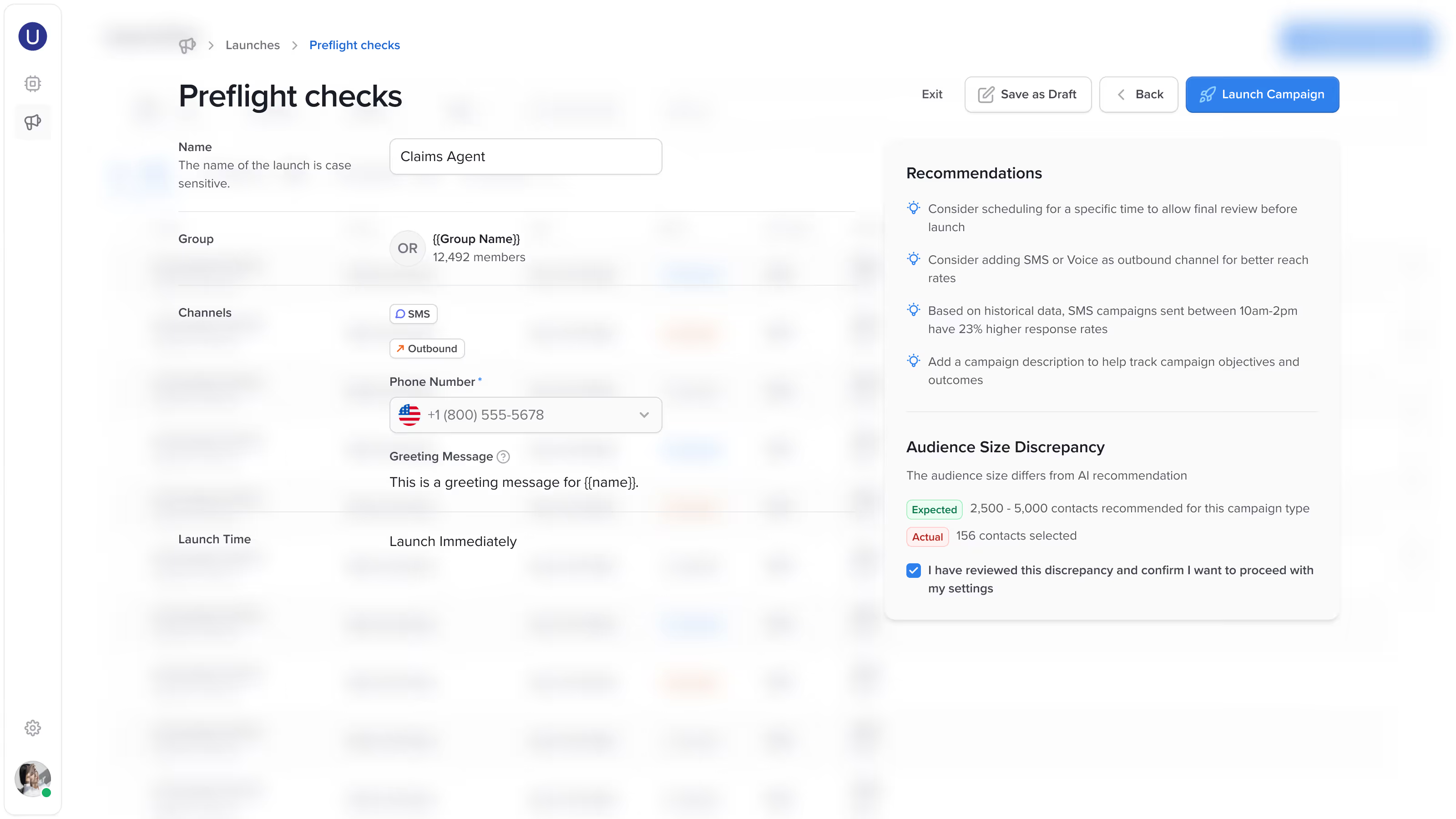
Purpose-built for regulated industries, delivering proactive outbound and inbound engagement — with compliance and auditability embedded into every interaction.

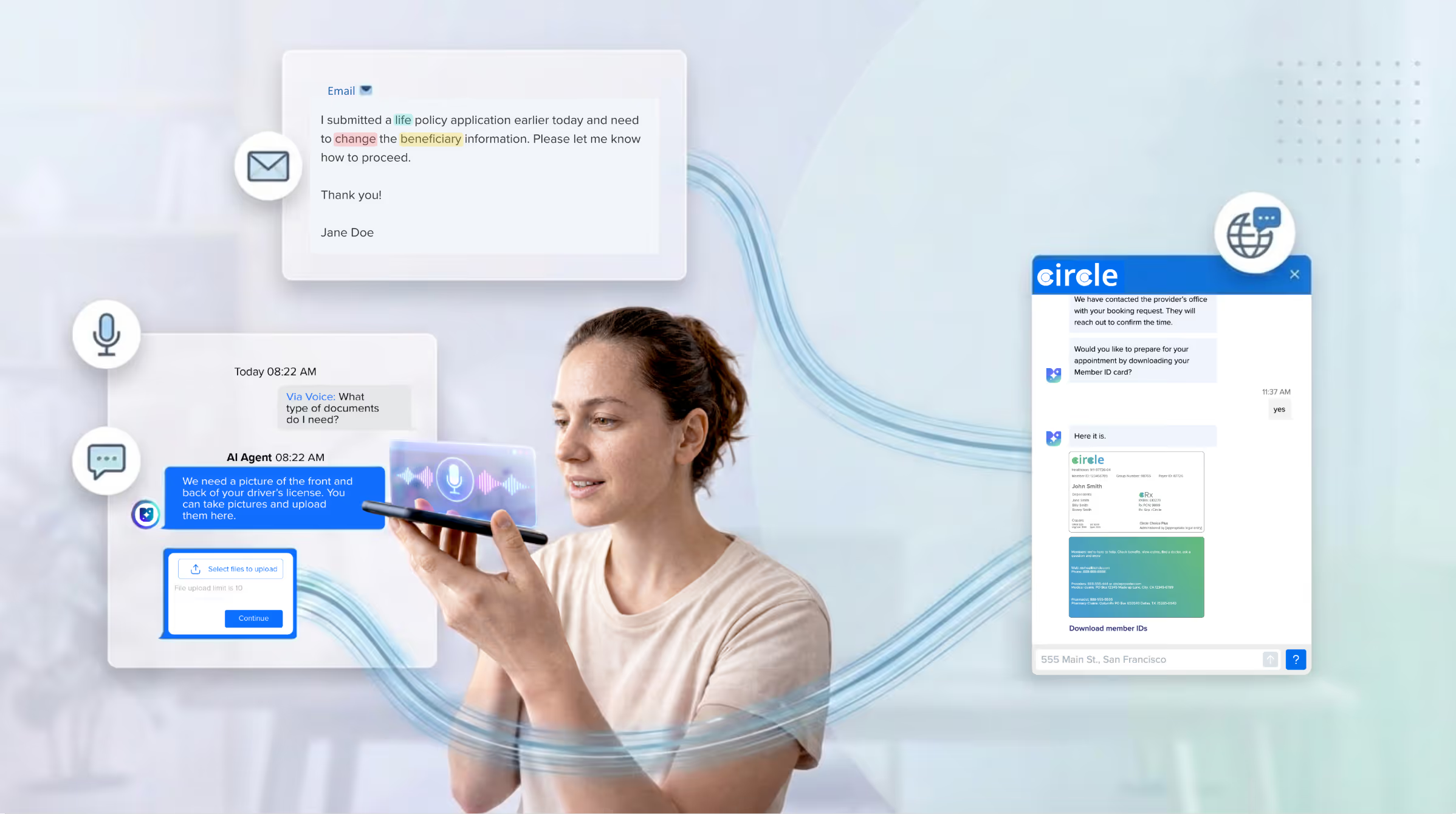
AI Agents That Deliver Better CX — Built on Trust


Trust-Native Architecture
Built-in governance embeds guardrails, policy enforcement, and human oversight directly into AI execution.
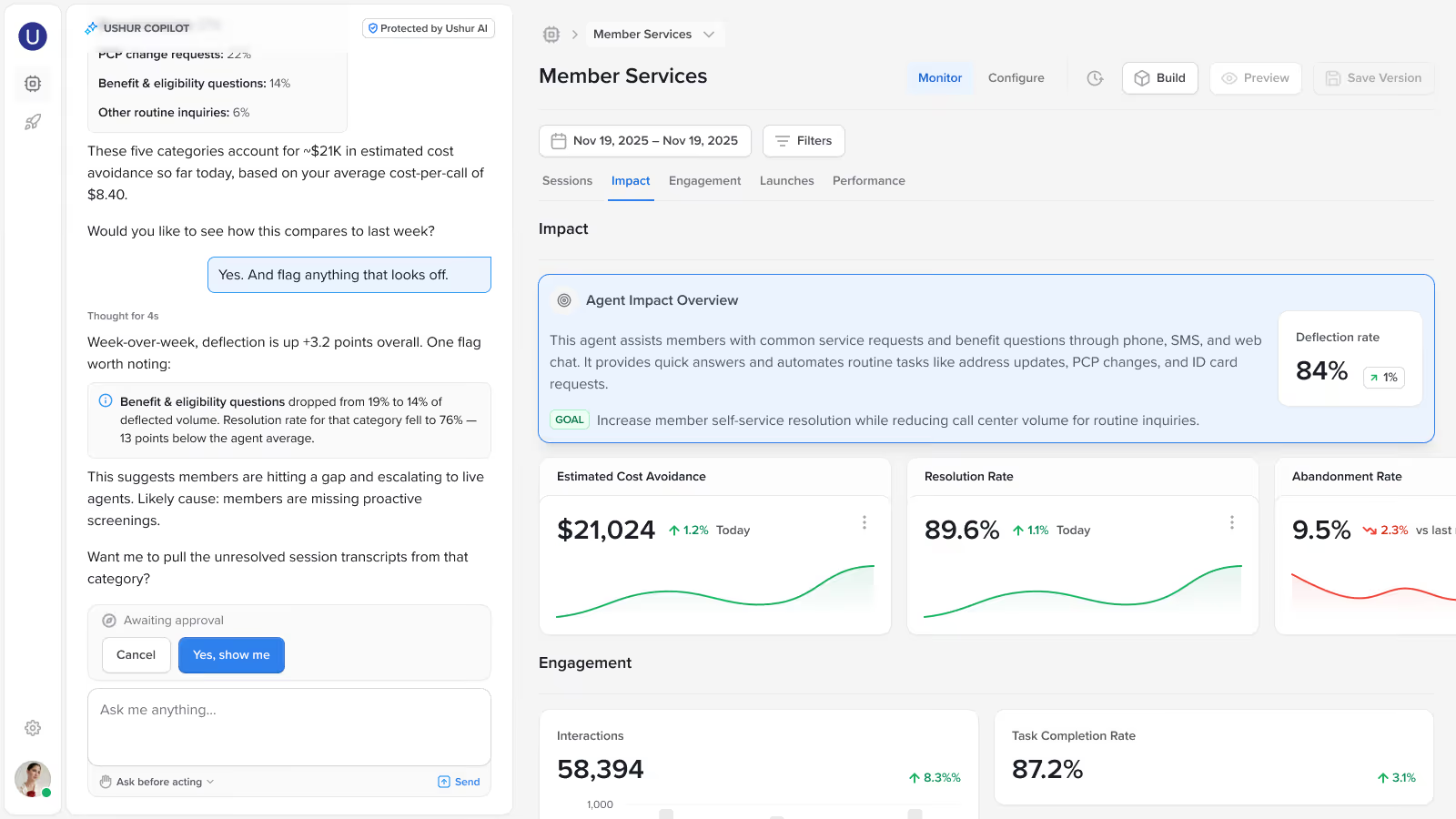
Maintain real-time visibility into agent behavior, reasoning, and performance.
Replay conversations end to end and generate regulator-ready records on demand.
Safeguard PHI, PII, and financial data with policy-aware segmentation and governed access.
The Ushur Agentic Platform
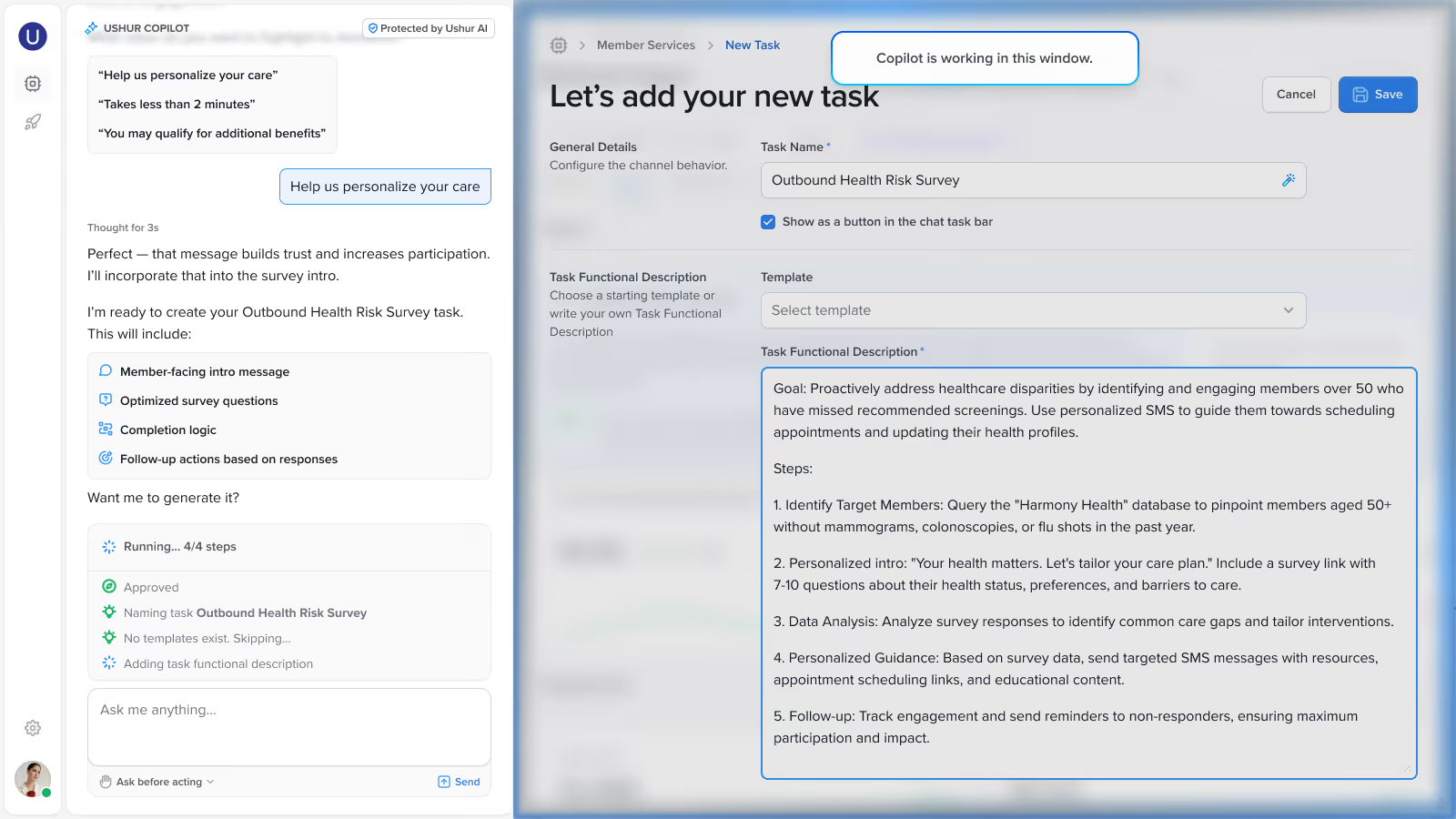
Enterprise AI Agents
AI agents that plan, reason, retrieve data, validate inputs, and resolve complex customer requests end-to-end — with built-in governance, human-in-the-loop safeguards, and full audit visibility.
One Platform. Endless Possibilities
A curated suite of Customer Experience Automation use cases built for regulated enterprises. Secure, compliant, and designed to resolve customer needs from start to finish
First Notice of Loss
Guide the Claimant through the process of reporting the death of a Policy Holder and filing a Claim.
Hospital discharge support
Support for inpatient to facility or home transitions to ensure safety and decrease readmissions
Digital ID Card
Securely deliver a digital copy of Member's Insurance ID Card upon request.
Medication reconciliation appointment setting
Education and scheduling of Medication Reconciliation
Member contact information collection / updates
Collection of cross-channel member contact information to support better communications
Extraction (Accidental Death & Dismemberment)
Extract Accidental Death and Dismemberment related keys required for underwriting from structured Census files, semi-structured Prior Year Plans, and unstructured email body.
Preventative wellness
Education and appointment setting for preventative wellness medications, immunizations and tests
Retail-to-mail conversion
Support for education and retail-to-mail conversion
Waitlisting
Proactive notifications of appointment availability for patients on wait lists
Payment Status
Provide Member with the current status of a payment on a Claim.
Payment Status
Provide Borrower with the current status of a payment made to their account.
Click-to-call or chat to speak to member service
Ability for service representatives to chat within Ushur journeys, and to warm call transfer to them
Digital consent
Ability for members to opt in to digital communications
Retail, mail order, 90-day medication refills
Support medication adherence with retail, mail order and 90-day refill request support
Shipping status updates
Shipment status updates
Click-to-call or chat to speak to other clinical staff member
Click-to-call or chat to speak to other clinical staff member when needed
Enrollment in mail order program and Rx transfers
Education on benefits of mail order delivery and Rx transfer support
Post care Surveys (NPS, CAHPs and HOS- like)
Post care and pharmacy visit surveys to understand experience gaps for proactive outreach and support as needed
Trailing Documents
Remind and support Applicant in securely uploading required supporting documents post Application.
Appointment reminder and rescheduling
Member appointment reminders for care management, provider appointments (any type), home health visits and more
Retail-to-mail conversion
Support for education and retail-to-mail conversion
Prior Authorization transparency support
Ability for members to receive push notices for, or make inquiries about, prior authorization status
Product Comparison
Support Applicants in finding Insurance Plan options that best fit their needs.
Support for shipping / delivery issues, returns and reshipment
Support for shipping / delivery issues, returns and reshipment
Vaccination reminders, education, appointment scheduling, and paperwork
Redetermination journey support (Medicaid)
Support for member retention with ongoing redetermination process education, support and services - until redetermination is complete
Transition of care support
Support for inpatient to facility or home transitions to ensure safety and decrease readmissions
Provider credentialing with Plan
Support for provider credentialing information submission and status updates
Proactive Rx status notifications
Proactive Rx status notifications (fill status, issues like prior auth)
Payment capture
Safe and secure collection of payment information (credit, debit, ACH) to pass to payment processing
Schedule Appointment
Schedule follow up call with Sales Representative with reminders and rescheduling.
Workplace Accommodations
Educate the Member on available workplace acommodations, reduced hours, and reassignment programs available through their employer.
Claim status, adjudication and payment updates
Ability for providers to inquire about claim status, adjudication and payments
Click-to-call or chat to speak to pharmacy staff
Ability for pharma representatives to chat within Ushur journeys, and to warm call transfer to them
Refill reminders and ordering facilitation
Refill reminders and ordering facilitation (including payment capture)
Prior Authorization transparency support
Ability for members to receive push notices for, or make inquiries about, prior authorization status
Preventative Wellness Care Gap Closure
Education, navigation support and appointment setting for any preventative wellness care gap (immunizations, cancer screenings)
Policy Review (KYC)
Remind and support Member in securely uploading required supporting KYC documents during Policy Review.
Trailing Documents
Remind and support Applicant in securely uploading required supporting documents post Application.
Policy Reinstatement
Guide the Policy Holder through re-instating a lapsed policy.
Incontinence education and support
Education and connectivity to support resources for incontenence
Product Comparison
Support for Applicants to find Insurance Plan options that best fit their needs.
Employer Onboarding
Guide the Broker / Employer through the information required from them to onboard them into the Carrier's core systems.
Return to Work
Confirm Claimant's Return to Work date as well as any supporting documentation from the doctor.
Schedule Appointment
Schedule follow up call with Sales Representative with reminders and rescheduling.
Certificate of Insurance (COI)
Respond to Policy Holder requests for copies of Certificate of Insurance (COI) with secure delivery of documents.
Loan Modification
Proactively reach out to delinquent Borrowers to educate them on eligible Loan Modification options available and support their decision.
Cost transparency and cost relief
Education on cost tranparency and cost relief options
Sales appointment setting and reminders
Member appointment setting with service or sales agents in support of their buying process
Provider roster directory updates
Ability for any provider to update their roster information for provider directory accuracy
Digital Consent
Ability for Members to opt in to digital communications.
Find a Primary Care doctor or Pediatrician
Support for finding a primary care doctor or pediatrician in network and setting appointment via click-to-call
Post-discharge information / education
Support for inpatient to facility or home transitions to ensure safety and decrease readmissions
Retail-to-mail conversion
Support for education and retail-to-mail conversion
Medication adherence
Medication Adherence (overcome barriers - cost, transportation, adverse effects)
Preventative wellness actions and care gap closure
Education, navigation support and appointment setting for any preventative wellness care gap (immunizations, cancer screenings)
Grievance filing and updates
Ability for members to understand and file Grievances, and receive status updates
Chronic Condition care gap closure
Education, navigation support and appointment setting for any chronic condition care gap (diabetes, CKD...)
Email Triage
Automatically triage incoming servicing emails to identify intent and respond to service requests.
Live Member Service chats and warm call transfers
Ability for service representatives to chat within Ushur journeys, and to warm call transfer to them
Claim Status
Provide Policy Holder with the current status of a Claim.
Medication adherence
Medication Adherence (overcome barriers - cost, transportation, adverse effects)
Shipping status updates
Shipment status updates
Maternal health navigation
Support for full maternity journeys with education, appointment setting, wellness and more
Chronic condition care navigation
Education, care management, navigation support and appointment setting for any chronic condition (diabetes, CKD...)
Escrow Review
Guide Borrower through shortfalls or excesses in their escrow account, the tax or insurance payments that led to the shortfall, and to securely accept payments for any shortfall.
First Notice of Injury
Guide the Claimant through reporting an injury and filing a Claim.
Annual Notice of Change (ANOC) FAQs
Proactive notifications and inquiry handling about Medicare Annual Notices of Change. Including FAQ support for top ANOC call drivers
Digital consent
Ability for members to opt in to digital communications
Chronic Condition care gap closure
Education, navigation support and appointment setting for any chronic condition care gap (diabetes, CKD...)
Issues and Complaints
Proactively detect issues and escalate them as tickets to reduce complaints and improve satisfaction.
Eligibility & benefits verification
Ability for providers and pharmacies to perform eligibilty and benefits verification at the member level
Sales appointment setting and reminders
Member appointment setting with service or sales agents in support of their buying process
Ongoing website, portal, & app adoption and utilization
Support for member ongoing utilization of website, traditional apps and portals
Experience and Net Promoter Score (NPS) surveys
Surveying capability for experiences and NPS scoring
Chronic Condition Care Gap Closure
Education, navigation support and appointment setting for any chronic condition care gap (diabetes, CKD...)
Extraction (Critical Illness)
Extract Critical Illness related keys required for underwriting from structured Census files, semi-structured Prior Year Plans, and unstructured email body.
Support for shipping / delivery issues, returns and reshipment
Support for shipping / delivery issues, returns and reshipment
Notification of lab and test results
Sharing of lab tests and results
Member contact information collection / updates
Collection of cross-channel member contact information to support better communications
Supporting Documents
Remind and support Claimant in securely uploading required supporting documents for a Claim.
Revenue cycle support - payment collection / auto-pay
Bill delivery with safe and secure collection of payment information (credit, debit, ACH) to pass to payment processing
SDOH resources (transportation, food)
Support for understanding and accessing SDOH resources such as nutrition, transportation
Experience and Net Promoter Score (NPS) surveys
Surveying capability for experiences and NPS scoring
Member warm welcome benefits education and literacy
Member welcome notifications that educate on plan benefits, deliver digital ID cards
Cardiac Disease care management and navigation
Year-round support for members with Cardiac Disease - including education, wellness, care gap closure, appointment setting
Surgery Confirmation
Collect detailed surgical information, including operative reports, discharge summaries, and post-operative recovery plans from the Claimant.
Schedule Appointment
Schedule follow up call with Sales Representative with reminders and rescheduling.
Care appointment reminders
Proactive care and provider appointment reminders with the ability to reschedule rather than no show (any provider type)
Care education (preventative care)
Notifications to educate on the importance of adult and pediatric preventative care, related appointment setting
Medication (Rx) reconciliation
Education and scheduling of Medication Reconciliation
Extraction (Short Term Disability)
Extract Short Term Disability related keys required for underwriting from structured Census files, semi-structured Prior Year Plans, and unstructured email body.
Transition of Care Support Readmission Avoidance
Support for inpatient to facility or home transitions to ensure safety and decrease readmissions
Census Transformation
Identify Census files in an inbound RFP and Transform the file to the standard format required by the Carrier and identify any issues.
Care education (chronic condition management)
Notifications to educate on the importance of chronic condition management, related appointment setting
Hardship Inquiry
Reach out to delinquent Borrowers with empathy to identify circumstances such as job loss, illness, divorce, deployment that may be eligible for relief measures.
Member information updates
Member information updates – including cross-channel contact details and change of insurance
Appeal filing and updates
Ability for members to understand and file Appeals, and receive status updates
New member welcome
New member welcome, overview of PBM supports and services, info gathering / sharing (including insurance ID card capture)
Follow-up appointment scheduling
Patient appointment setting support with reminders and ability to reschedule
Don’t see the use case you are looking for? Let’s talk about your unique requirements. Schedule time with our team to explore what is possible.